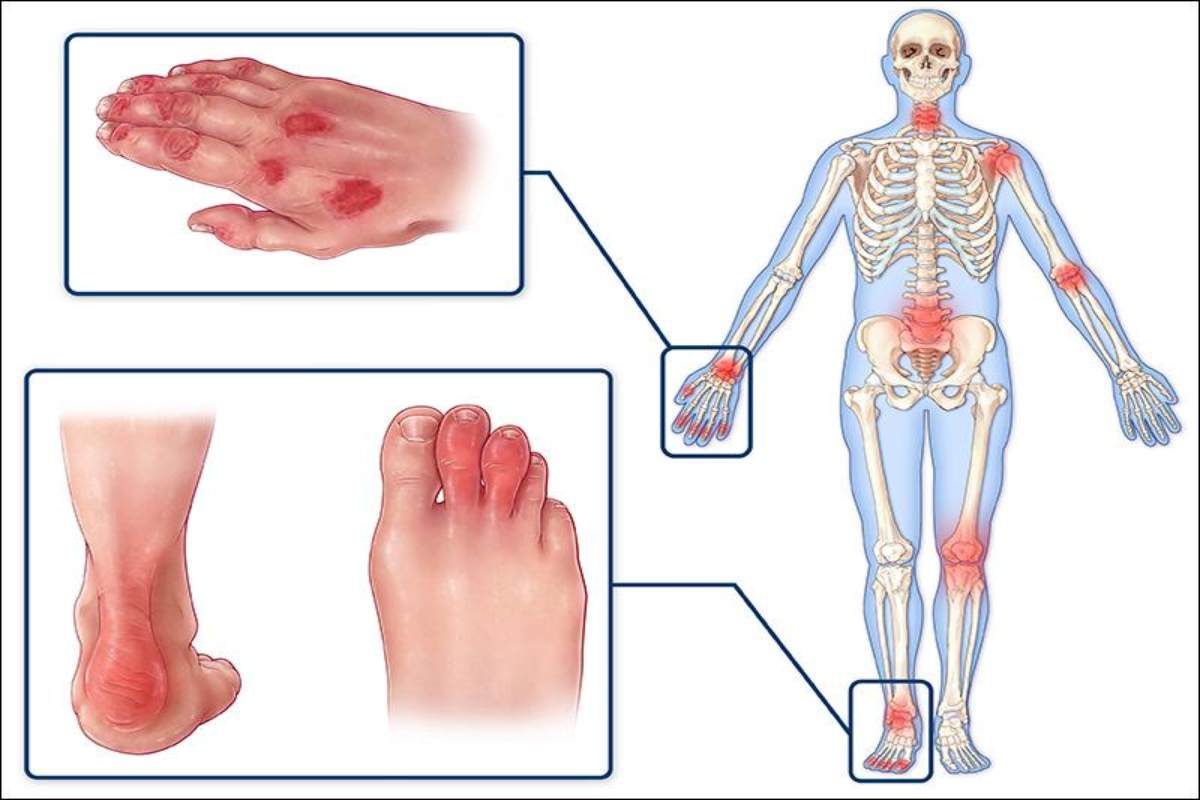
Psoriatic arthritis is a condition where joint pain and swelling happen along with a skin problem called psoriasis. It usually affects people who already have psoriasis, which causes itchy, scaly patches on the skin and scalp. You can learn more about it in our guide on psoriasis.
This condition doesn’t look the same for everyone. Some people may have mild symptoms, while others can experience more serious joint problems over time. It can affect one or several joints in the body.
If you or someone close to you has been diagnosed with psoriatic arthritis, it’s normal to have questions. Understanding the symptoms, causes, and treatment options can make it easier to manage daily life.
Table of Contents
What are the Symptoms of Psoriatic Arthritis (PsA)?
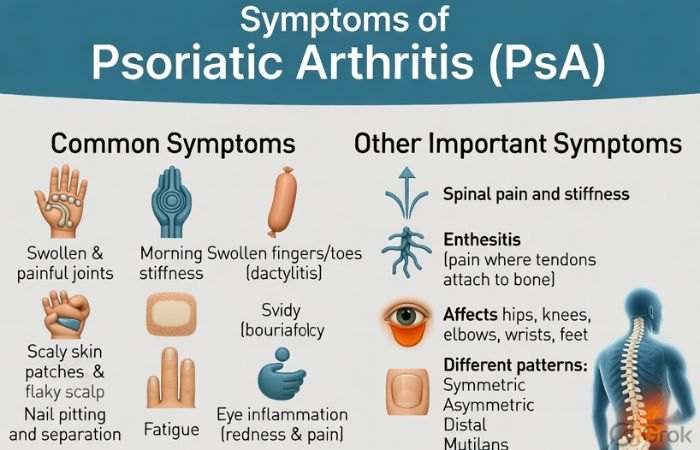 The symptoms of PsA are different for each person. They can range from mild to severe. Sometimes your condition goes into remission, and you feel better for a while. In other cases, your signs may get worse. And also, Your symptoms depend on the type of PSA.
The symptoms of PsA are different for each person. They can range from mild to severe. Sometimes your condition goes into remission, and you feel better for a while. In other cases, your signs may get worse. And also, Your symptoms depend on the type of PSA.
Common Symptoms of PSA Include:
swollen and painful joints on one or both sides of the body
- morning stiffness
- swollen fingers and toes
- sore muscles and tendons
scaly patches on the skin, which may get worse when joint pain flares up
- flaky scalp
- fatigue
- nail pitting
- separation of the nail
- eye redness
- eye pain (uveitis)
- fatigue
Spondyloarthritis PSA, in particular, can also cause the following symptoms:
Spinal pain and stiffness
- Pain, swelling and weakness in your:
- hips
- knees
- pegs
- feet
- elbow
- hands
- wrists
- other joints
swollen fingers or toes
Symmetrical PA affects five or more joints on both sides of the body. Asymmetric PA affects fewer than five joints, but they can be on opposite sides.
Psoriatic arthritis mutilans is a rare method of arthritis that distorts the joints. It can shorten affected fingers and toes. Distal PA causes pain and swelling in the end joints of the fingers and toes.
Symptoms at a Glance
| Symptom | Description |
| Joint pain | Swelling and stiffness |
| Skin patches | Red, scaly areas |
| Nail changes | Pitting or separation |
| Fatigue | Low energy levels |
| Eye issues | Redness, pain |
What Reasons Psoriatic Arthritis (PsA)?
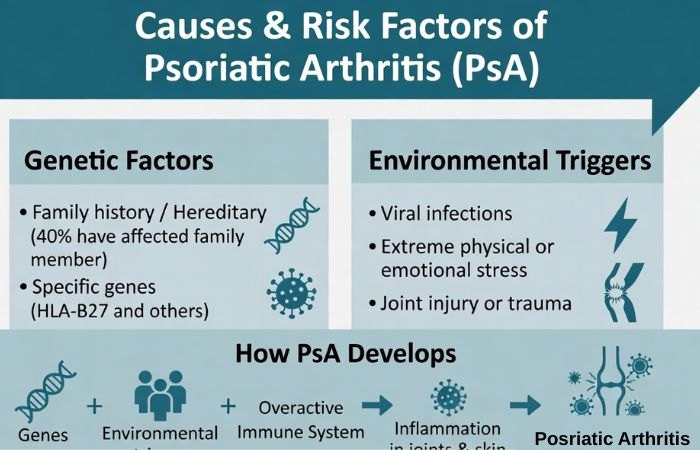
In PsA, your immune system spells your joints and skin. The Doctors don’t know for sure what causes these attacks. They think it comes from a combination of genes and environmental factors.
According to the Centers for Disease Control and Prevention (CDC), psoriatic arthritis is linked to both genetic and environmental factors.
PSA runs in families. About 40% of people with the disease have one or more family members with PsA. Something in the environment often triggers the disease in people with a tendency to develop PSA. It could be a virus, extreme stress or an injury.
How is Psoriatic Arthritis (PsA) Treated?
PSA treatment aims to recover symptoms, such as rash and joint swelling.
Trusted Source guidelines published in 2018 recommend the “treat the target” approach based on a person’s individual preferences. Although A specific treatment goal and how to measure progress are determined, a doctor works with you to select treatments.
You have many different treatment options. Although, A typical action plan will include one or more of the following:
Nonsteroidal Anti-Inflammatory Drugs (NSAIDs)
These medicines help control joint pain and swelling. Although, Over-the-counter (OTC) options include ibuprofen (Advil) and naproxen (Aleve). If over-the-counter options aren’t effective, your doctor may prescribe NSAIDs in higher doses.
- If used incorrectly, NSAIDs can cause:
- stomach irritation
- stomach bleeding
- heart attack
liver and kidney damage
Disease-Modifying Antirheumatic Drugs (DMARDs)
These drugs reduce inflammation to prevent joint damage and slow the progression of PA. And also, they can be administered by various routes, including orally, by injection or by infusion.
The most commonly prescribed DMARDs include:
- methotrexate (Trexall)
- leflunomide (Arava)
- sulfasalazine (Azulfidine)
Apremilast (Otezla) is a newer DMARD that is taken by mouth. Although, It works by blocking phosphodiesterase 4, an enzyme involved in inflammation.
Side effects of DMARDs include:
- Liver damage
- bone marrow suppression
- lung infections
- steroids
PsA, they are usually injected into the affected joints. These drugs can reduce inflammation. Although, Side effects include pain and a slight risk of joint infection.
Immunosuppressants
Medications such as azathioprine (Imuran) and cyclosporine (Gengraf) calm the overactive immune response in PSA, especially for psoriasis symptoms. They are not used as often now that TNF-alpha inhibitors are available. Although they weaken the immune response, immunosuppressants can increase the risk of infections.
Topical Treatments
Creams, gels, lotions, and ointments can relieve an itchy rash. Although, These actions are available over the counter and by prescription.
Options include:
- The anthralin
- calcitriol or calcipotriene
- salicylic acid
- steroid creams
- Tazarotene, which is a vitamin A derivative
- Light therapy and other medications for PsA
Latest Treatments for Psoriatic Arthritis
Recent advancements have improved how psoriatic arthritis is treated. Doctors now focus on controlling inflammation early and preventing joint damage.
New & Advanced Treatment Options:
- Biologic drugs (TNF inhibitors) – target specific immune responses
- IL-17 & IL-23 inhibitors – newer therapies for skin + joint symptoms
- JAK inhibitors – oral drugs that reduce inflammation
- Personalized treatment plans – based on disease severity
These treatments help reduce flare-ups and improve long-term quality of life.
Quick Summary of Psoriatic Arthritis
| Factor | Details |
| Type | Autoimmune disease |
| Main Cause | Immune system dysfunction |
| Affected Areas | Joints, skin, nails |
| Common Symptoms | Joint pain, swelling, skin patches |
| Severity | Mild to severe |
| Treatment | NSAIDs, DMARDs, Biologics |
You may also find helpful information in our related articles on rheumatic diseases